How much can change in a year. It was just a year ago, on June 15, 2017, that a Presidential Advisory from the American Heart Association was published on the topic of dietary fats and cardiovascular disease. The panel of experts provided definitive recommendations based on an extensive literature review to limit foods high in saturated fats, as well as to avoid coconut oil. A news release from the American Heart Association summarized the major findings as:
“The advisory reports that:
Randomized controlled trials that lowered intake of dietary saturated fat and replaced it with polyunsaturated vegetable oil reduced cardiovascular disease by approximately 30 percent –similar to that achieved by cholesterol-lowering drugs, known as statins.
Prospective observational studies in many populations showed that lower intake of saturated fat coupled with higher intake of polyunsaturated and monounsaturated fat is associated with lower rates of cardiovascular disease.
Several studies found that coconut oil — which is predominantly saturated fat and widely touted as healthy — raised LDL cholesterol in the same way as other saturated fats found in butter, beef fat and palm oil.
Replacement of saturated fat with mostly refined carbohydrate and sugars is not associated with lower rates of CVD.”
It seemed that the advice on dietary fats from a panel of experts was clear, and unity in terms of educating public to avoid heart disease was at hand. The public would learn to cut back on dairy, cheese and meats of all kinds, avoid replacing those foods with processed foods rich in the “deadly whites” of refined flour and sugar, and have the option to replace them with polyunsaturated fats, whole grains, and legumes.
Sadly, unity on this topic did not develop after June of 2017. The conversation took an ugly turn likely due to financial or career conflicts with the AHA statements. The most outrageous of the reports in response to the AHA Advisory was titled “Is the American Heart Association a Terrorist Organization”. Geary claimed that the AHA was even more effective than ISIS at terrorism! This piece of irresponsible reporting was sadly reposted, liked or retweeted by some prominent figures like Aseem Malhotra, MD, a cardiologist in the UK, and celebrity author Nina Teicholz. If you wanted more outrage last summer your got it by reading the post asking whether the AHA or coconut oil was more likely to kill you? Why did Teicholz retweet such an untenable media headline grabber linking this advisory to the “AHA killers”? Equally poor judgement was exhibited in a piece entitled “Why Coconut Oil Won’t Kill You but Listening to the American Heart Association Might!” posted on social media. The accompanying meme with the quote and a spoon of the white oil in dispute was shared or liked on Twitter by some prominent leaders in medicine.
The irony of the AHA effort, and the ugly backlash, is that a year later, almost to the day, another consensus statement was published in the British Medical Journal. This article was authored by Dr. Nita Fohouri of University of Cambridge, Ronald Krauss, M.D. of the Oakland Research Institute, Gary Taubes, journalist, and Walter Willett, M.D., Harvard Professor at the TH Chan School of Public Health. This seems an unusual pairing of academic researchers and a journalist, with both Dr. Krauss and Mr. Taubes known for repeatedly praising diets high in animal fat content.
The article referred to the scientific work of Ancel Keys, Ph.D. and was refreshing in that it avoided adding inappropriate terms like demonic or satanic to refer to Dr. Keys long and honored career (adjectives used by many authors since Dr. Keys died at age 100 in 2004). The Diet-heart Hypothesis was described as:
Box 1
Diet-heart hypothesis
The seemingly simple diet-heart hypothesis was first proposed by nutritionist Ancel Keys in the early 1950s. The hypothesis outlined a sequence of relationships in which a fatty diet elevates serum cholesterol levels, leading to atherosclerosis and myocardial infarction. The focus of the hypothesis soon shifted from the total fat consumed in the diet to the more nuanced idea that saturated fats should be replaced by polyunsaturated fats and the benefits of replacing animal fats with vegetable fats were advocated. Total cholesterol as the atherogenic biomarker was later replaced by cholesterol subfractions: the cholesterol in low density lipoproteins and high density lipoproteins, and serum levels of triglycerides. That science, too, has continued to evolve in complexity with further research
The article went on to review data dietary fats summarized in their Box 2 as:
Box 2
Dietary fats and their food sources
· Dietary fats are mostly triglycerides, with each triglyceride molecule containing three fatty acids on a glycerol backbone
· The structure and function of dietary fatty acids can vary greatly depending on chain length (6–24 carbon units); number of double bonds — saturated (with no double bonds), monounsaturated, or polyunsaturated; and whether the double bonds are in a cis (same side) or trans (opposite side) position
· Polyunsaturated fats with double bonds that are 3 carbon atoms or 6 carbons from the n-terminal end of the fatty acid (n-3 or n-6, respectively) are considered essential — that is, they must be obtained from the diet because they are not synthesised in the body. Both have important structural and physiological functions
· Different fatty acids have distinct biochemical properties and can therefore produce different metabolic and physiological effects with different clinical manifestations, such as cardiovascular, neurological, or other
Food sources of dietary fats
· Food sources of individual fatty acids vary within each class. For instance, within the omega 3 polyunsaturated fatty acid class, alpha linolenic acid comes from plants, including some nuts and seeds such as walnuts and linseed, whereas eicosapentaenoic acid and docosahexaenoic acid come mostly from fish and other marine sources
· Many food sources contain different types of fatty acids. For example, olive oil is a good source of monounsaturated fatty acids but also contains saturated and polyunsaturated fatty acids in smaller proportions. Animal products are rich in saturated fats but some also contain large proportions of monounsaturated and polyunsaturated fatty acids
The group did bring up the “hot” topic of whether adding coconut oil to the diet was recommended and concluded, in agreement with the AHA Presidential Advisory, that caution was appropriate:
Although a recent report suggests that coconut oil compared with butter results in a more favourable lipid profile (lower LDL, higher HDL cholesterol), and compared with olive oil was equivalent in lipid effects,56 further research is needed in large long term trials and current recommendations on caution about use should be upheld.1
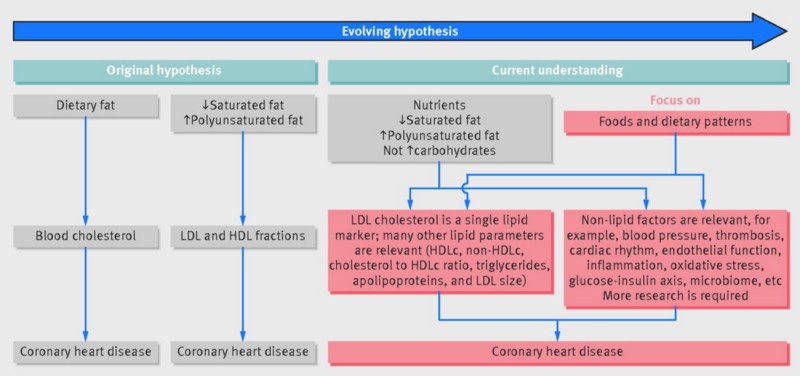
Finally, a summary of key messages was provided (along with a flow chart of the group’s recommendations which is at the start of this article):
Key messages
· For cardiovascular health, substantial evidence supports the importance of the type of fat consumed, not total fat intake, and the elimination of industrially produced trans fats
· Much of the evidence suggests that the risk of coronary heart disease is reduced by replacing saturated fat with polyunsaturated fats (including plant oils) but not when carbohydrate is the replacement nutrient
· Controversies remain about long term health effects of specific plant oils and of high fat, low carbohydrate diets, and research is needed to resolve these
· The focus of dietary advice must be on the consumption of foods and overall dietary patterns, not on single nutrients
All in all, if you were tough enough to ride out the blasphemous response to the AHA Presidential Advisory of June 15, 2017, calm waters have reappeared in June of 2018 and include some unexpected recruits like Taubes and Dr. Krauss. The 2018 article would have been a better consensus had the term carbohydrates, not a food group but a macronutrient class, been differentiated into foods rich in refined carbohydrates and processing versus foods rich in complex carbohydrates like legumes and vegetables. The noisy and ugly group of 2017 that responded to the AHA Presidential Advisory has been silent in terms of this new consensus document, perhaps unable to criticize some of their own “peers” like Taubes and Krauss, or perhaps actually enlightened that the data again supports the long term health benefits of inserting foods with PUFAs, including plants oils, in place of foods rich in saturated fats, including coconut oil. Eat food, not too much, mostly plants, and not dripping in coconut oil or butter would seem to ring true again.

